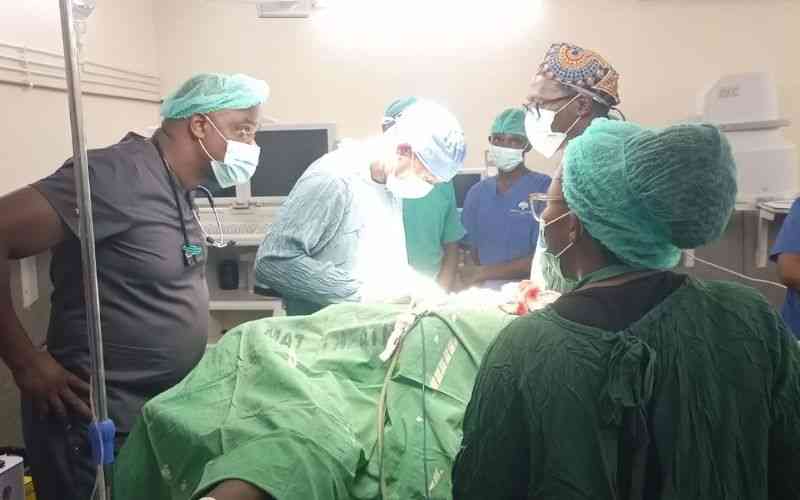
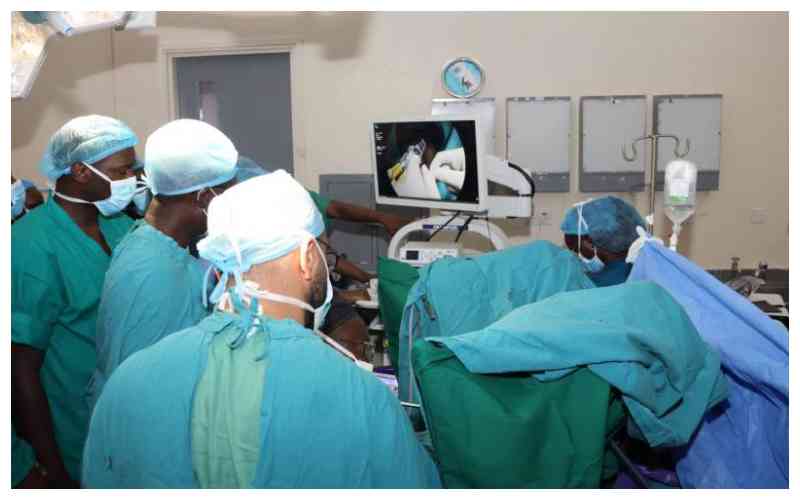
Health PS Ouma Oluga during a visit to Kenyatta National Hospital Oncology centre on World Cancer Day 2026. [Collins Oduor, Standard]
The conversation around cancer in Kenya has never been more urgent.
For many, a cancer diagnosis is not only a medical challenge but a life-altering event, bringing emotional, social, and financial burdens that extend far beyond hospital walls.
From the moment abnormal cells begin to grow uncontrollably to the long and expensive treatment journey, the reality of living with cancer is profound.
Yet, amidst these challenges, stories of resilience, survival, and hope shine a light on what is possible with early detection, timely treatment, and robust support systems.
According to Dr Afrin Shaffi, Gynaecological Oncologist at Nairobi West Hospital, cancer treatment in Kenya is expensive in multiple aspects.
“From the initial diagnostics to treatment, supportive care, and follow-up, patients bear enormous financial and emotional burdens. Cancer care is not just a medical intervention it is a whole-life consideration for both patients and their families,” she explains.
- WHO says four out of every 10 cancer cases are preventable
- Cancer and HIV remain among leading causes of death among Kenyan women today
- MPs call for overhaul of cancer treatment access and funding
- Nairobi targets system gaps as late cancer diagnoses strain care capacity
Keep Reading
“Cancer in its simplest terms, is an abnormal growth of cells. Normally, cells grow, divide, and die in a controlled way. When this process goes awry, cells multiply uncontrollably, forming tumors. This can occur anywhere in the body from the head, breast, uterus, or skin,” Dr Shaffi says.
Cancers may be solid tumors, such as breast or cervical cancers, or liquid tumors, like leukemias and lymphomas. The type, location, and behavior of the cancer determine the approach to treatment and prognosis.
According to Dr Shaffi, not all cancers arise randomly. Many are influenced by a combination of genetics, lifestyle, and environmental factors. “Some cancers are hereditary,” she explains. “BRCA1 and BRCA2 gene mutations increase the risk of breast and ovarian cancers. Lynch syndrome predisposes individuals to uterine and colon cancers. These gene abnormalities often run in families, making awareness and genetic counseling critical for early intervention.”
“Human papillomavirus (HPV) is responsible for most cervical cancers and can also affect other reproductive organs. Some cancers may develop spontaneously without clear triggers, which is why regular screening and health vigilance are crucial.”
Dr Rose Munge, Paediatrician and Paediatric Haematologist-Oncologist at Kenyatta University Teaching, Research, and Referral Hospital (KUTRRH), adds that in children, cancer may not always have a clear cause.
Pediatric cancers such as leukemia or certain solid tumors often appear without identifiable risk factors. Early diagnosis, she emphasizes, is the single most important determinant of outcomes.
Survival rates
Early detection of cancer is critical because it increases survival chances. Cervical and breast cancers are among the few that can be detected before they fully develop, offering patients the opportunity for preventive treatment.
“Screening with HPV DNA tests or Pap smears allows abnormal cervical cells to be identified early, before they become malignant,” Dr Shaffi explains.
“Breast cancer can be detected through clinical examinations, mammograms, and ultrasounds. Detecting cancer early gives patients more treatment options and improves survival rates. Symptoms like abnormal bleeding, persistent bloating, fatigue, or unexplained weight loss should never be ignored.”
Understanding how far the disease has spread is critical, and this is where cancer staging comes in. “Stage one cancers are usually localized to one area,” Dr Shaffi explains.
“Stage two and three involve adjacent tissues, and stage four represents metastasis, where cancer spreads to distant organs. The earlier the stage at diagnosis, the more treatment options are available and the better the likely outcome.”
Imaging techniques such as CT scans, MRI, and PET scans help oncologists determine the extent of disease.
Biopsies, sometimes combined with immunohistochemistry, are used to confirm cancer type and guide treatment.
“Accurate staging is critical because it informs the best approach, whether surgery, chemotherapy, radiotherapy, or targeted therapy,” Dr Shaffi adds.
Treatment in Kenya is determined by the type and stage of cancer, as well as the patient’s overall health and available resources.
Options include surgery to remove localized tumors, chemotherapy to kill cancer cells or slow their growth, radiotherapy using high-energy radiation to destroy cancer cells, targeted therapies which attack specific characteristics of cancer cells, and immunotherapies that enhance the body’s immune system to fight the disease.
“The financial burden of cancer in Kenya is immense. Costs begin with diagnostics, including biopsies, imaging, and specialized tests, which can run into tens of thousands of shillings. “Then come treatment costs,” Dr Shaffi explains.
“Surgery, chemotherapy, radiotherapy, and newer therapies like immunotherapy are expensive. Supportive care, such as blood transfusions, dietary needs, counseling, and even transportation to treatment centers, adds to the burden. For instance, immunotherapy can cost between Sh70,000 and Sh450,000 per dose administered every three weeks, sometimes for years.”
Indirect costs also include lost income for patients and caregivers. “A patient may be unable to work during treatment, while a caregiver may need to take extended leave,” Dr Shaffi observes.
“These financial pressures often cause patients to delay care or forego treatment entirely.”
Cancer is the third leading cause of death in Kenya after infectious and cardiovascular diseases.
According to GLOBOCAN 2022, Kenya reports 44,726 new cases annually and 102,152 five-year prevalence cases. Women are disproportionately affected, with breast and cervical cancers leading incidence and mortality.
Breast cancer accounts for 23.3 per cent of female cases, emphasizing the importance of mammograms and self-examinations, while cervical cancer is the second most common, with 5,845 new cases and 3,600 deaths annually.
Despite being largely preventable through HPV vaccination and early screening, many women are diagnosed late due to limited access, stigma, and lack of awareness.
Bone marrow transplants
To address this, the government launched the National Cervical Cancer Elimination Action Plan 2026–2030, a five-year strategy to accelerate prevention, screening, and treatment.
Pediatric cancer care is another critical area. On January 23, the National Cancer Institute of Kenya convened a stakeholder meeting in Nairobi to establish a National Childhood Cancer Registry. The registry aims to standardize pediatric cancer reporting, strengthen data systems for early diagnosis, and support research and long-term patient outcomes.
“Accurate diagnosis in children is the first hurdle,” Dr Munge explains. “Without it, treatment cannot begin. Advanced therapies like bone marrow transplants are limited to a single center in Kenya, making early and correct diagnosis even more critical.”
Beyond statistics, cancer is about human experience, fear, hope, and resilience. Emmy Angeeyo, 29, noticed a tiny bump on her nipple in 2020 while preparing to welcome a baby. Her concern grew when her baby struggled to breastfeed. A biopsy confirmed breast cancer.
“I was devastated,” Emmy recalls. “I thought cancer was a death sentence. I had lost my cousin within a year, so I believed I wouldn’t survive.” Today, Emmy is a survivor. “I no longer let cancer control me. My condition is stable, and I take medications to manage my hormones. I am a survivor.”
Scholastica Gichuhi, 41, ignored a lump in her breast for four years until it began oozing foul discharge. Diagnosis revealed cancer that had spread to her lungs. “Friends disappeared, stigma was overwhelming, and finances were scarce. But I have survived two years of chemotherapy and am now in my third year of maintenance therapy. Each day, I thank God for another day,” says Scholastica.
Experts stress that cancer is not always a death sentence. “Early detection improves survival dramatically,” Dr Shaffi notes. “Even advanced cancers can be managed with the right treatment and support.” Dr Munge advises, “The earlier the intervention, the higher the chances of a positive outcome.”
Despite progress, significant gaps remain in Kenya’s cancer care. Late diagnosis sees over 70 per cent of patients presenting at advanced stages. Access to specialized care is limited, particularly in rural areas, and high treatment costs often remain prohibitive.
Cancer is a growing public health challenge in Kenya. With over 44,000 new cases annually and 32,000 deaths, the need for awareness, early detection, and affordable care has never been more pressing.
“With timely intervention, cancer can be managed successfully, and survival is possible,” Dr Shaffi says.
On World Cancer Day, the message is clear: knowledge, vigilance, and compassion are powerful tools in the fight against cancer.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.